
Our system detects bacterial transmission in real time, giving hospitals the visibility to intervene before infections occur.
Healthcare-associated infections (HAIs) remain one of the most costly and persistent risks in hospital operations, and the clinical stakes are rising. Antimicrobial-resistant pathogens are increasing rapidly in U.S. hospitals, reflected by the CDC’s recent announcement of >460% surge since 2019 in deadly bacterial superbugs containing the NDM resistance gene (1).
Despite dedicated Infection Prevention teams, a staggering 90% of in-hospital transmission goes undetected (2-4) - not from lack of effort, but because transmission is largely invisible without real-time sequencing. At the same time, the investigations that do occur are often misdirected. When suspected outbreaks are later sequenced, fewer than 10% prove to be genetically linked, consuming scarce resources (3). Without tools to detect transmission as it begins, IP teams lack the visibility to intervene early. The result is substantial cost to hospitals, payers, and patients, including longer stays, strained capacity, regulatory penalties, reputational risk, and patient harm.
NGD IP has made it cost effective and operationally practical to track transmission with our automated sample preparation, real time sequencing capabilities and immediate bioinformatic analysis; NGD IP’s system makes transmission detection low-cost and actionable, enabling infection prevention teams to intervene quickly.
-
1 CDC report finds sharp rise in dangerous drug-resistant bacteria: NDM-CRE infections increased >460% in the United States, 2019–2023. Centers for Disease Control and Prevention (CDC), September, 2025.
2 Longitudinal genomic surveillance of MRSA in the UK reveals transmission patterns in hospitals and the community. Coll et al., Sci Transl Med, 2017.
3 Whole-Genome Sequencing Surveillance and Machine Learning of the Electronic Health Record for Enhanced Healthcare Outbreak Detection. Sundermann, et al. Clinical Infectious Diseases, 2022.
4 Clinical Implementation of Routine Whole-Genome Sequencing for Hospital Infection Control of Multi-drug Resistant Pathogens. Harris, et al. Clinical Infectious Diseases, 2023.
How Our System Can Benefit Your Hospital
With every averted transmission event, hospitals deploying real-time detection can achieve: earlier outbreak identification, more targeted interventions while avoiding wasted resource on false alarms, reduction in average length of stay, measurable downstream cost savings and reputational protection Improved patient outcome and experience.
Modeled health-system analyses show potential ROI greater than 20:1 when applied at operational surveillance scale.
-
For financial modeling, we apply a conservative 20– 25% reduction in transmission-related infections, materially below reductions observed in best-in-class programs, recognizing that impact depends on baseline rates and operational execution.
-
Preventing these infections avoids hundreds to thousands of inpatient bed-days annually, driving a measurable reduction in average LOS and improving capacity.
-
Proactive genomic evidence strengthens documentation, supports defensible reporting, and reduces exposure to penalties tied to hospital-acquired conditions.
-
Genomic confirmation significantly reduces false transmission investigations and manual tracing, improving Infection Prevention team effiency. This allows Infection Prevention teams to shift effort from weeks-late outbreak refutation to real-time intervention when transmission is detected.
The NGD System
Providing actionable transmission insights available within ~24hrs of isolate readiness using NGD200 and EpiAssist

NGD System Core Capabilities

Fully automated sample preparation with NGD200
Makes routine sequencing feasible without specialized personnel. It prepares up to 48 bacterial samples in a single run, completing the workflow required to move samples to sequencing.
In about 4 hours, the system delivers 48 barcoded samples ready to be loaded onto the sequencer, making routine in-hospital transmission detection operationally achievable.

Automated and validated bioinformatics
Rapidly determines whether samples sequenced overnight are linked to one another or to prior isolates, enabling earlier intervention before transmission becomes a larger outbreak.
The highly scalable system, developed over 8 years, is so optimized that it can compare today’s samples against thousands sequenced in the previous year and generate transmission detection reports soon after sequencing is completed.
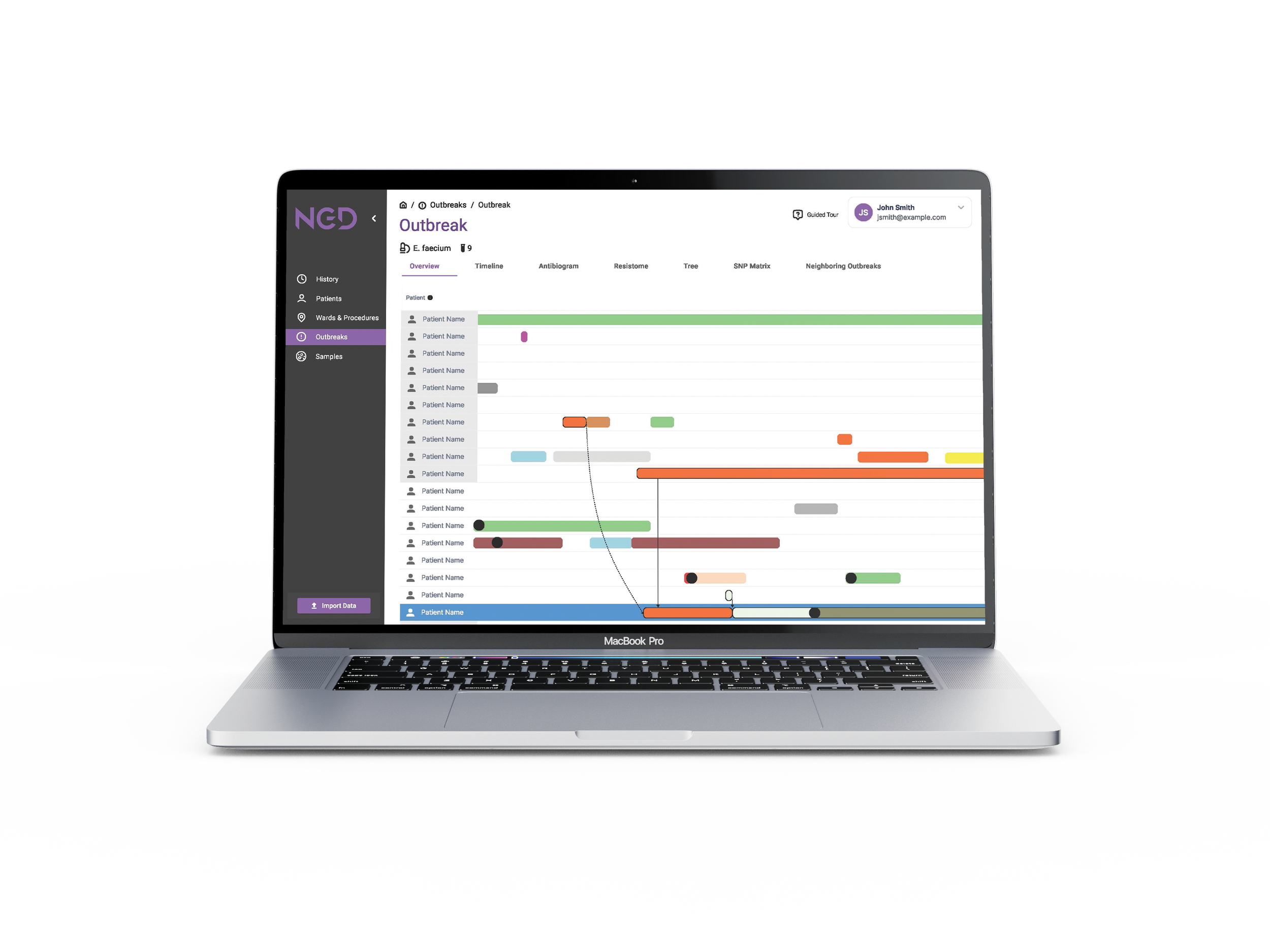
Interactive epidemiologic user interface: NGD EpiAssist
Operating in a HIPAA-compliant manner and entirely within the hospital firewall, EpiAssist builds an interactive timeline of patients, wards, locations, procedures, and shared caregivers.
It assists Infection Prevention teams in identifying likely root causes and documenting interventions, dramatically reducing the time required for outbreak investigation.
